The intricacies of therapeutical management have brought to light a pervasive issue – drug-related problems (DRP). A substantial portion of DRPs stems from drug prescribing challenges. These can span from inaccurate dosing to frequency mismanagement, exacerbating known allergies, or triggering drug-drug interactions (DDIs). The prevalence of polypharmacy, particularly in geriatric patients, adds another layer of complexity. Swiss studies underscore that polypharmacy prevalence increases significantly with age. Deciphering the nuances of DDIs becomes imperative, as they contribute to overall hospital admissions in the elderly population, with a notable percentage of adverse drug reactions (ADRs) being DDI-related.
Pharmacokinetic and Pharmacodynamic Drug-Drug Interactions
The realm of drug interactions encompasses both pharmacokinetic (PK) and pharmacodynamic (PD) aspects. PK DDIs manifest when a perpetrator drug influences the absorption, distribution, metabolism, or elimination (ADME) of a victim drug. Conversely, PD interactions occur when two drugs directly interact on the same target without altering ADME parameters. The consequences of DDIs can range from mild side effects to severe, life-threatening events or syndromes
Drug Metabolism and Transport
Drug metabolism unfolds through phase I and phase II reactions, primarily mediated by Cytochrome P-450 (CYP450) enzymes. Phase II reactions involve conjugation processes facilitated by enzymes like UDP-glucuronosyltransferases (UGTs). Simultaneously, membrane transporters play a pivotal role in drug absorption, distribution, and elimination. Uptake transporters (OATPs, OATs, OCTs) and efflux transporters (P-gp, BCRP) are key players in influencing drug efficacy
Genetic Polymorphism of Drug Metabolizing Enzymes and Transporters
Understanding the genetic basis of drug metabolism is crucial. CYP enzymes, especially CYP1A, CYP2C-D-E, and CYP3A, exhibit significant polymorphism, influencing drug metabolism. Genetic variations contribute to 20–30% of the variability in drug response. Enzymes like UGTs and various transporters, such as P-gp and BCRP, also exhibit genetic polymorphism, adding another layer of complexity.
Predictive Models
The evolution of computational tools has paved the way for predictive models in clinical pharmacology. Quantitative structure-activity relationships (QSAR), quantitative systems pharmacology (QSP), and pharmacokinetic modeling (PK modeling) offer insights into drug behavior. A notable advancement is physiologically based pharmacokinetic (PBPK) modeling, providing a dynamic, bottom-up approach that considers individual variability and factors like genetics, diseases, and co-treatments
System Property Building to PBPK Models
PBPK models, endorsed by regulatory authorities, present a mechanistic framework for predicting drug exposure and response across diverse populations. Initiatives like PK-Sim and platforms like SimCYP® and GastroPlus® have democratized the application of PBPK models.
The Persistent Challenge
Despite strides in understanding drug metabolism and disposition, DDIs remain a challenge. Predicting vulnerability to DDIs is paramount for averting adverse effects. A knowledge base, collating PBPK predictions from literature, underscores the need for continued investigation into the interplay between DDIs and genetic variations in metabolic enzymes and transporters. The quest for a predictive model that encompasses intrinsic and extrinsic factors persists, providing a holistic approach to personalized medicine and safer drug administration.
Study DOI: 10.3389/fphar.2021.708299
Engr. Dex Marco Tiu Guibelondo, B.Sc. Pharm, R.Ph., B.Sc. CpE
Editor-in-Chief, PharmaFEATURES

Subscribe
to get our
LATEST NEWS
Related Posts

Drug Discovery Biology
Proteolytic Rewriting: Engineering Controlled Absence of Pathogenic Protein Persistence
Targeted protein degradation transforms drug therapy by engineering the cellular machinery to erase, rather than merely inhibit, pathogenic proteins.

Drug Discovery Biology
Open Nucleotides: Grant-Driven Infrastructure for Equitable mRNA Vaccine Manufacturing
By developing accessible cap analogs and RNA raw materials, Hongene Biotech, guided by David Butler’s expertise in nucleotide chemistry and supported by the Gates Foundation, is reshaping the molecular infrastructure that underpins global mRNA vaccine equity.
Drug Discovery Biology
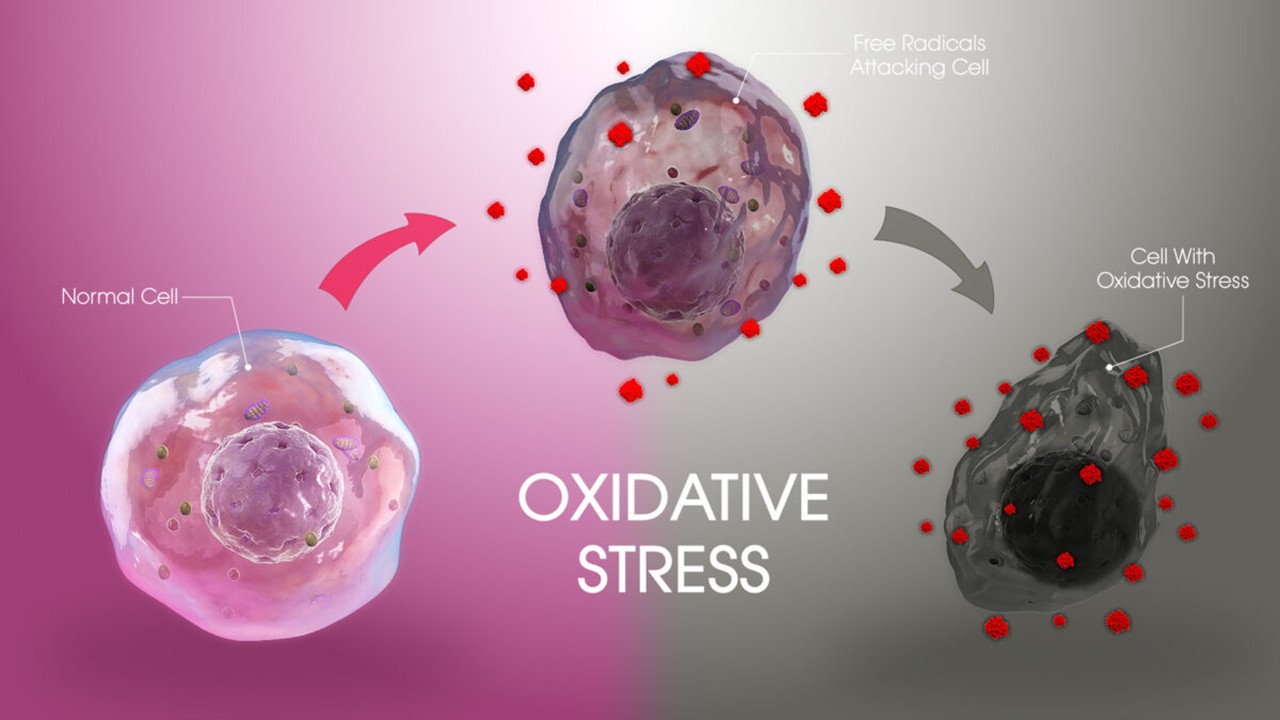
Redox Messengers: How Endogenous Gasotransmitters Rewire Vascular Biology to Resist Age-Driven Oxidative Stress
Gasotransmitters provide a biologically sophisticated means of counteracting age-related oxidative stress and preserving vascular resilience.
Drug Discovery Biology
Aptamer Signal Dynamics: Engineering Nucleic Acid Recognition Systems for High-Fidelity, Multi-Modal Biosensing
Aptamers redefine biosensing by pairing programmable molecular recognition with versatile transduction strategies capable of detecting clinically relevant biomarkers with exceptional fidelity.
Read More Articles
Algorithmic Therapeutics: Artificial Intelligence Reshaping Biotech Drug Discovery and Product Development
Artificial intelligence is transforming biotech by making therapeutic discovery less like screening for luck and more like engineering across molecules, biologics, and delivery systems.
Factory Logic: Modular Pharmaceutical Manufacturing Enabling Rapid Drug Production and Continuous Innovation
Modular pharmaceutical factories transform drug manufacturing into a continuously evolving technological system capable of integrating new therapies, processes, and production innovations without disrupting regulated operations.
Spatial Collapse: Pharmacologic Degradation of PDEδ to Disrupt Oncogenic KRAS Membrane Localization
PDEδ degradation disrupts KRAS membrane localization to collapse oncogenic signaling through spatial pharmacology rather than direct enzymatic inhibition.
Neumedics’ Integrated Innovation Model: Dr. Mark Nelson on Translating Drug Discovery into API Synthesis
Dr. Mark Nelson of Neumedics outlines how integrating medicinal chemistry with scalable API synthesis from the earliest design stages defines the next evolution of pharmaceutical development.
Zentalis Pharmaceuticals’ Clinical Strategy Architecture: Dr. Stalder on Data Foresight and Oncology Execution
Dr. Joseph Stalder of Zentalis Pharmaceuticals examines how predictive data integration and disciplined program governance are redefining the future of late-stage oncology development.







